Keloid scars, sometimes referred to simply as 'keloids', are scars that overgrow, eventually becoming larger than the original wound that caused them in the first place. In this edition of the Jobskin® blog, we'll be looking in more detail at keloids and ways in which they can be managed.
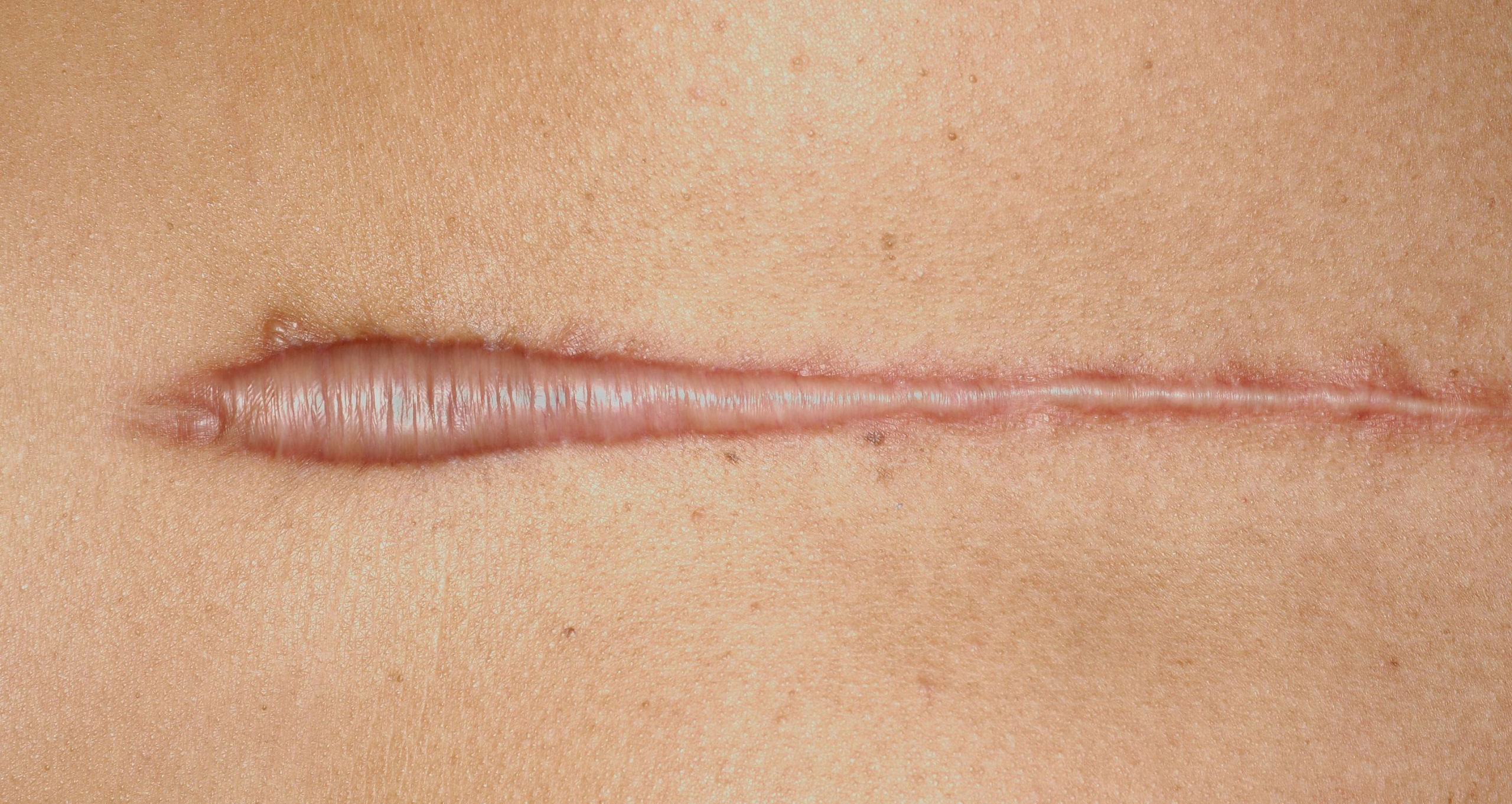
Coined over two centuries ago, the original term for a keloid scar was 'chéloïde'. The word derives from the Greek 'chele', meaning 'crab's claw', referring to the way in which keloids grow sideways into the skin.
When a wound heals, scar tissue forms. Though the texture and colour may be different to the surrounding healthy skin, it usually fades and flattens after treatment and/or time, sometimes becoming raised and slightly thick. This is known as a 'hypertrophic' scar. Keloids are different from hypertrophic scars in three major ways:
- They can develop after skin damage that could be considered minor, such as that caused by acne. They can even develop without any noticeable skin trauma and are then referred to as 'spontaneous keloids'
- They spread or 'grow' beyond the original area of skin that has been damaged
- They can on occasion be permanent
It is not completely understood what causes keloids but they appear to occur due to an overproduction of collagen. The number of people who develop keloids is a minority of the general population but they have been found to be more common in some ethnic groups, including Hispanics, Asians, and Africans.
Keloids are not usually hereditary but, according to the British Association of Dermatologists, some studies have suggested that 5-10% of Europeans with keloids have 'a positive family history.' There are also a number of risk factors affecting the likelihood of a person developing keloid scars:
- They are most likely to occur following a burn injury, acne scars, infected wounds, or significantly tightened skin during the healing process
- They are most common on the lower limbs, neck, chin, shoulders, sternum, and upper chest. Keloids also commonly occur after ear piercing
- They are more likely to affect those who have previously had a keloid
- They are more common between puberty and the age of 30 years
- They can appear or get larger during pregnancy
Though there is currently no known cure for keloids, a variety of treatment methods are available including surgery, steroids, compression, cryotherapy, and laser therapy. Silicone dressings and gels have also been shown to help reduce the thickness of keloids and make their colour paler and less noticeable.
At Jobskin®, we offer silicone therapy products in the form of both sheet and gel: ScarFX® and ScarSil® respectively. For more information about these products, please refer to the Jobskin® website.
NB - information in this article taken from British Association of Dermatologists website at https://www.bad.org.uk/for-the-public/patient-information-leaflets/keloids